News
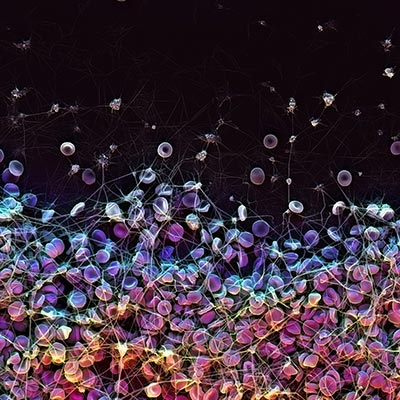
This Scanning Electron Microscope (SEM) image shows how red blood cells coagulate to form a blood clot, which is a common and life-threatening risk associated with the use of implanted medical devices. (image by James Weaver/Wyss Institute at Harvard University)
Cambridge, Mass. – October 12, 2014 – From joint replacements to cardiac implants and dialysis machines, medical devices enhance or save lives on a daily basis. However, any device implanted in the body or in contact with flowing blood faces two critical challenges that can threaten the life of the patient the device is meant to help: blood clotting and bacterial infection.
A team of Harvard scientists and engineers may have a solution. They developed a new surface coating for medical devices using materials already approved by the Food and Drug Administration (FDA). The coating repelled blood from more than 20 medically relevant substrates the team tested—made of plastic, glass, and metal—and also suppressed biofilm formation in a study reported in Nature Biotechnology. But that’s not all.
The team implanted medical-grade tubing and catheters coated with the material in large blood vessels in pigs, and it prevented blood from clotting for at least eight hours without the use of blood thinners such as heparin. Heparin is notorious for causing potentially lethal side-effects like excessive bleeding but is often a necessary evil in medical treatments where clotting is a risk.
“Devising a way to prevent blood clotting without using anticoagulants is one of the holy grails in medicine,” said senior author Donald Ingber, the Judah Folkman Professor of Vascular Biology at Harvard Medical School and Boston Children’s Hospital, Professor of Bioengineering at Harvard School of Engineering and Applied Sciences (SEAS), and Founding Director of Harvard’s Wyss Institute for Biologically Inspired Engineering.
The idea for the coating evolved from SLIPS, a pioneering surface technology developed by coauthor Joanna Aizenberg, Amy Smith Berylson Professor of Materials Science at SEAS and Professor in the Department of Chemistry and Chemical Biology. She is also a core faculty member at the Wyss Institute, leading the Adaptive Materials Technologies platform there. SLIPS stands for Slippery Liquid-Infused Porous Surfaces. Inspired by the slippery surface of the carnivorous pitcher plant, which enables the plant to capture insects, SLIPS repels nearly any material it contacts. The liquid layer on the surface provides a barrier to everything from ice to crude oil and blood.
“Traditional SLIPS uses porous, textured surface substrates to immobilize the liquid layer whereas medical surfaces are mostly flat and smooth—so we further adapted our approach by capitalizing on the natural roughness of chemically modified surfaces of medical devices,” said Aizenberg, who leads the Wyss Institute’s Adaptive Materials platform. “This is yet another incarnation of the highly customizable SLIPS platform that can be designed to create slippery, non-adhesive surfaces on any material.”
The researchers developed a super-repellent coating that can be adhered to existing, approved medical devices. In a two-step surface-coating process, they chemically attached a monolayer of perfluorocarbon, which is similar to Teflon. Then they added a layer of liquid perfluorocarbon, which is widely used in medicine for applications such as liquid ventilation for infants with breathing challenges, blood substitution, eye surgery, and more. The team calls the tethered perfluorocarbon plus the liquid layer a Tethered-Liquid Perfluorocarbon surface, or TLP for short.
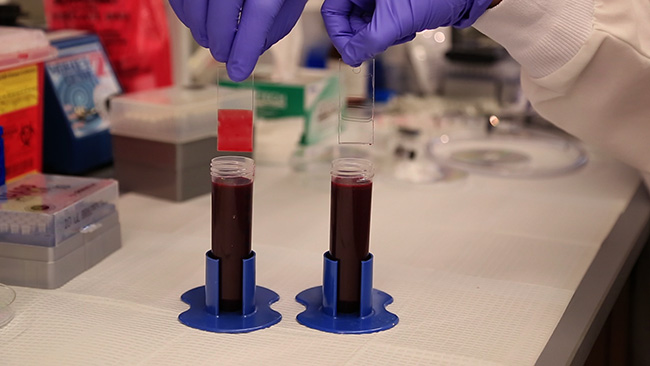
These glass slides were dipped in blood to demonstrate the effectiveness of the TLP coating. While blood sticks to the untreated slide on the left, the TLP-treated slide on the right emerges entirely clear. (photo by Seth Kroll/Wyss Institute at Harvard University)
In addition to working seamlessly when coated on more than 20 different medical surfaces and lasting for more than eight hours to prevent clots in a pig under relatively high blood flow rates without the use of heparin, the TLP coating achieved the following results:
- TLP-treated medical tubing was stored for more than a year under normal temperature and humidity conditions and still prevented clot formation.
- The TLP surface remained stable under the full range of clinically relevant physiological shear stresses, or rates of blood flow seen in catheters and central lines, all the way up to dialysis machines.
- It repelled the components of blood that cause clotting (fibrin and platelets).
- When bacteria called Pseudomonas aeruginosa were grown in TLP-coated medical tubing for more than six weeks, less than one in a billion bacteria were able to adhere. Central lines coated with TLP significantly reduce sepsis from Central-Line Mediated Bloodstream Infections (CLABSI). (Sepsis is a life-threatening blood infection caused by bacteria, and a significant risk for patients with implanted medical devices.)
Out of sheer curiosity, the researchers even tested a TLP-coated surface with a gecko—the superstar of sticking whose footpads contain many thousands of hair-like structures with tremendous adhesive strength. The gecko was unable to hold on.
“We were wonderfully surprised by how well the TLP coating worked, particularly in vivo without heparin,” said one of the co-lead authors, Anna Waterhouse, a Wyss Institute Postdoctoral Fellow. “Usually the blood will start to clot within an hour in the extracorporeal circuit, so our experiments really demonstrate the clinical relevance of this new coating.”
While most of the team’s demonstrations were performed on medical devices such as catheters and perfusion tubing using relatively simple setups, they say there is a lot more on the horizon.
“We feel this is just the beginning of how we might test this for use in the clinic,” said co-lead author Daniel Leslie, a Wyss Institute Staff Scientist, who aims to test it on more complex systems such as dialysis machines and ECMO, a machine used in the intensive care unit to help critically ill patients breathe.
Reflecting the strong collaborative model of the Wyss Institute, the cross-disciplinary team included researchers representing the Wyss Institute, SEAS, Harvard Medical School, and Boston Children’s Hospital whose specialties range from hematology to immunology, surface chemistry and materials science.
Ingber said the technology "could become a new paradigm for implantable medical devices, extracorporeal circuits, and more.”
The project was funded by the Defense Advanced Research Projects Agency (DARPA) and the Wyss Institute for Biologically Inspired Engineering at Harvard University.
Topics: Materials, Bioengineering
Cutting-edge science delivered direct to your inbox.
Join the Harvard SEAS mailing list.
Scientist Profiles
Joanna Aizenberg
Amy Smith Berylson Professor of Materials Science and Professor of Chemistry & Chemical Biology
Press Contact
Paul Karoff